Your cart is currently empty!
Author: digital
-

Adani’s Empty Promises: Unraveling a Potential Investment Mirage
In the high-stakes world of international business and politics, promises can be as ephemeral as smoke—and sometimes just as deceptive. The case of Gautam Adani, an Indian billionaire facing serious fraud allegations, exemplifies how grand proclamations of economic transformation can mask potentially corrupt practices. What begins as a tantalizing tweet about massive U.S. investments quickly unravels under scrutiny, revealing a narrative of political maneuvering, dubious claims, and potential systematic deception.
Last November Gautam Adani, one of the world’s richest men, was charged with fraud and bribery by the US Department of Justice for an alleged scheme to bribe Indian Government officials and defraud U.S investors. Since the indictment numerous Republican representatives have expressed outrage at their own government for daring to hold Adani accountable. These representatives are MAGA diehards and their criticisms of the DOJ are predictable, weak – and sometimes bizarre. Their letters claim that George Soros is secretly controlling the Department of Justice. They also claim that the US has no jurisdiction to investigate bribery. The most outrageous claim, however, is that Adani is poised to bring thousands of jobs and billions in investment to the United States.
It goes without saying that “creating jobs and investment” is not a defense in a bribery trial. However, the idea that Adani is on the verge of a spending spree creating thousands of U.S. jobs might make some Americans think that dropping charges could be a good idea. Who doesn’t want to unleash a tidal wave of prosperity and employment? However, the evidence is pretty clear: Americans waiting to get hired by Adani will be waiting a long long time.
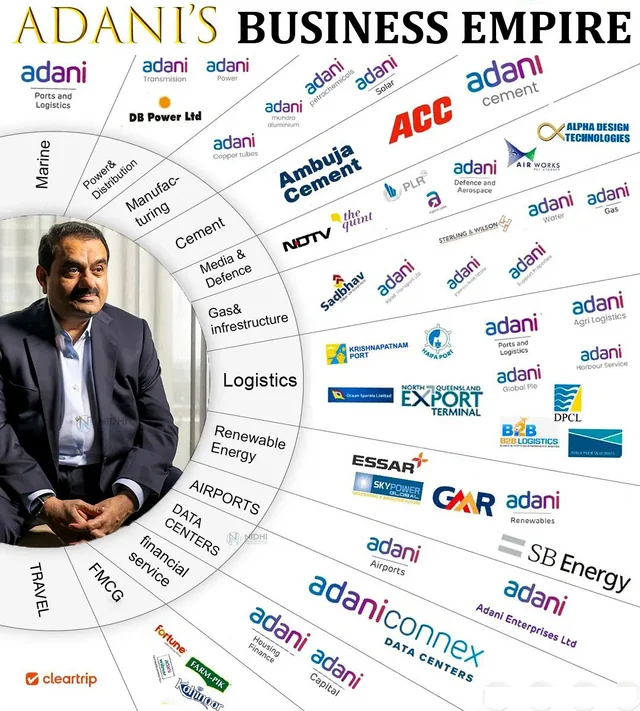
Adani is founder and Chairman of the Adani Group is a multinational conglomerate involved in everything from ports to energy production to infrastructure development. Much of Adani’s financial success comes from lucrative government contracts granted by India’s ruling party.
The Promised Investment
The massive U.S. investment plan has been most explicitly detailed in a single tweet by Gautam Adani himself – shortly after the election of Donald Trump. In his tweet Adani offered congratulations to the new American President and committed to leverage “global expertise and invest $10 billion in US energy security, aiming to create up to 15,000 jobs.” Beneath that commitment Adani added an A.I. generated image of an industrial utopia replete with busy ports, trainlines, tractors, multiple jet planes and the sun streaming through conjoined US and Indian flags.
Legal Challenges and Political Maneuvering
Seven days later, in New York, Adani and other executives were indicted on charges related to millions of dollars in alleged bribes, and all talk of new U.S. investment disappeared as Adani stock plunged. However, Adani and his American allies soon got to work hiring multiple American law firms and lining up lobbyist support. Soon after, MAGA-aligned Republican representatives were openly declaring that the charges were unfair. Following a State visit by Indian Prime Minister Narendra Modi to the White House, the Financial Times announced that the “investment plan” was potentially back on – as long as the charges against Adani are dropped.
Lack of Substantial Evidence
It’s easy to understand why Adani and his MAGA allies want people to believe that a wave of jobs and prosperity will magically appear if he’s not charged. However, if you take away a 40-word tweet, the evidence for a massive job creation plan gets very thin indeed. While Sudipta Bhattacharya holds the impressive title of CEO – Adani Group North America, it’s unclear whether the Group even has an actual office in the US. Mail is directed to an address in Jersey City. Adani’s one business that actually is registered in the United States, Adani Solar USA, has used a variety of addresses on government forms – including what appears to be a residential home in Dallas – for their lobbying registrations.

Hindenburg Research titled their 2023 Report on Adani, “The Largest Con In Corporate History”. The title speaks for itself, detailing a long history of allegations of money laundering, theft of taxpayer funds and corruption. The report quotes one insider with knowledge of Adani’s business practices saying, “[A]s an investor why would you invest with Adani Group? Because you know that the stock is inflated, you know that they cannot be trusted…. looking at the business, I mean it’s a house of cards, it´s all fueled on debt… I think that this is really how brazen this is happening. It´s like, almost like the Russia of the late 90s, that´s what´s happening.” Any American expecting Adani to magically create 15,000 jobs would do well to remember these words.
i Times of India, Feb 11, 2025 “Adani indictment: 6 Congressmen writes to Attorney General”
iii Link
iv Link
v Link
-
Adani Group and Dharavi: Corporate Expansion, PoliticalConnections, and Community Displacement in Mumbai
Adani-ACORN-White-Paper-v1.9-1
For nearly two decades, ACORN International has supported organizations working in Dharavi, a
community of millions in the heart of Mumbai. The report details the dangers facing residents
in the face of a re-development contract granted to the Adani Group, questions about the
granting of the contract and the history of the Adani Group including the serious concerns about
corporate governance and criminal indictments. -

Living Rent Members in Troglen Secure Victory: Action Against Damp, Mould, and Unsafe Living Conditions Leads to Immediate Results!
Living Rent members at Sanctuary Housing in Troglen banded together out of concern for damp and mould in their homes, clogged gutters, and woodlice on the balconies. Residents banded together and took action- submitting a petition with over 70 signatures demanding a meeting with Sanctuary’s Housing Director, and marching on the central office. Within a week, results were secured, just in time for Christmas!
-

ACORN Honduras Wraps Up 2024 with Strong Connections: Evaluating Progress and Expanding Support for Children’s Rights into 2025.
This December, ACORN Honduras did an end-of-year evaluation of their activities and accomplishments in support of rights for children, and spent time connecting with local community centers to expand and deepen their network. Kicking off 2025 right!
-

ACORN Peru Wraps Up 2024 with Solidarity and Support: Soup Kitchens, Art Workshops, and New Partnerships.
In December, ACORN Peru focused on solidarity actions and cultural activities to close the year out strong, including a soup kitchen in Calaralas, art workshops for local students, and building a new relationship with a community in San Jose, who are requesting help negotiating with local authorities.
-

A Community Voice Celebrates Advocacy & Honors Local Leaders at Annual Awardees Dinner and Christmas Party.
A Community Voice hosted their annual Awardees Dinner and Christmas party, where members of the community were honored for the advocacy to advance the causes of the working people of Louisiana. Honorees included Inez Barnes, Diane Adams, Rev. Richard S Bell Sr, and Louisiana State Representative Matthew Willard.
-

ACORN Canada Celebrates a Year of Victories – People Power Prevails!
ACORN Canada had a year full of successes, and as December came to a close, many took time out to celebrate the ACORN community and all it has done. ACORN Ottawa hosted a “People Power Party” where over 50 members gathered to honor the hard-fought wins and progress made throughout 2024, including stopping multiple renovictions, launching the Eco-Tenant platform, and forming new tenant unions—so much to celebrate!
-

ACORN Brighton Reflects on 2024 Wins & Gears Up for 2025 Campaign on Affordable Bus Fares.
ACORN Brighton held their final meeting of the year, and used the time to reflect on the accomplishments of 2024, as well as gear up for their first big campaign of 2025- advocating for affordable bus fares.
-

ACORN Ontario Organizes for Rent Control While Ottawa Tenants Demand Anti-Renoviction Bylaw
ACORN Canada had a busy month, with over 100 ACORN Ontario members organizing critical next steps for full rent control in the face of imminent early elections. Ottawa ACORN amassed over 70 ACORN members and tenants from across the city in front of city hall to show city council how important and urgent an anti-renoviction bylaw is to the tenants in this city! When we fight together, we win!
-

CATU Ireland: Supporting the Fight Against Unfair Evictions – Join the Fundraiser!
CATU Ireland ended a year of incredible wins by launching a fundraiser raising money for their tireless advocacy for blocking unfair evictions. As the housing situation in Ireland continues to deteriorate under current leaderships, their work is even more essential. When we band together, we can make protect each other!
